Ergocalciferol (Vitamin D2)
Ergocalciferol (vitamin D2) is a secosteroid produced by UV irradiation of ergosterol in fungi and plants, serving as one of two major forms of vitamin D supplementation, though with lower potency and shorter duration of action compared to cholecalciferol (vitamin D3).
Ergocalciferol (Vitamin D2) is a fat-soluble vitamin derived from plants and fungi that must undergo two hydroxylation steps in the body to become biologically active. It promotes calcium absorption, supports bone health, and plays roles in immune function, cell growth, and inflammation reduction. While commonly prescribed for vitamin D deficiency, research suggests D3 (cholecalciferol) may be more effective at raising and maintaining serum vitamin D levels.
Overview
Ergocalciferol (vitamin D2) is a secosteroid formed when ergosterol, a sterol found in fungal cell membranes and some plant tissues, is exposed to ultraviolet B radiation (wavelengths 280–315 nm). This photochemical reaction, which mirrors the production of vitamin D3 (cholecalciferol) from 7-dehydrocholesterol in human skin, was first characterized in the 1930s and led to the widespread fortification of foods with D2 to combat rickets. Structurally, ergocalciferol differs from cholecalciferol by the presence of a double bond between C22 and C23 and a methyl group at C24 on the side chain, differences that significantly affect its metabolism and potency.
Like cholecalciferol, ergocalciferol undergoes two hydroxylation steps to become biologically active. The first occurs in the liver via CYP2R1 and CYP27A1, producing 25-hydroxyvitamin D2 (25(OH)D2, or ercalcidiol), and the second in the kidneys via CYP27B1, yielding the active hormone 1,25-dihydroxyvitamin D2. However, the structural differences in the side chain result in weaker binding to vitamin D-binding protein (DBP), faster hepatic catabolism, and reduced affinity for the vitamin D receptor (VDR). Multiple comparative studies and meta-analyses have concluded that D2 is approximately 30–50% less effective than D3 at raising and maintaining serum 25(OH)D levels, particularly with intermittent dosing regimens.
Despite its lower potency, ergocalciferol retains clinical relevance as the only non-animal-derived form of vitamin D, making it suitable for vegan populations. It is available in prescription-strength formulations (typically 50,000 IU capsules) widely used for the treatment of vitamin D deficiency. UV-exposed mushrooms (shiitake, maitake, and white button) represent a meaningful dietary source of D2. Current clinical guidance from the Endocrine Society generally favors cholecalciferol for routine supplementation but recognizes ergocalciferol as an acceptable alternative when D3 is not suitable.
Mechanism of Action
Vitamin D Receptor Activation
Ergocalciferol (vitamin D2) is a secosteroid derived from the fungal sterol ergosterol via UVB-induced photolysis. Upon ingestion, it undergoes two sequential hydroxylations: first in the liver by CYP2R1 and CYP27A1 to form 25-hydroxyvitamin D2 (25(OH)D2), then in the kidney by CYP27B1 (1-alpha-hydroxylase) to yield the active hormone 1,25-dihydroxyvitamin D2 (1,25(OH)2D2). This active metabolite binds the intracellular vitamin D receptor (VDR), a nuclear transcription factor that heterodimerizes with retinoid X receptor (RXR) and engages vitamin D response elements (VDREs) on target gene promoters (PMID: 17634462).
Calcium & Phosphate Homeostasis
The VDR-RXR complex upregulates intestinal expression of TRPV6 (calcium channel), calbindin-D9k (intracellular calcium transporter), and PMCA1b (basolateral calcium ATPase), collectively increasing transcellular calcium absorption. In the kidney, 1,25(OH)2D2 enhances calcium reabsorption in the distal tubule via TRPV5. It also modulates phosphate handling by regulating NaPi-IIb cotransporters in the intestine and NaPi-IIa/IIc in renal proximal tubules (PMID: 21118827).
Bone Metabolism
In osteoblasts, VDR activation stimulates production of RANKL (receptor activator of NF-kB ligand), which binds RANK on osteoclast precursors to drive their differentiation and bone resorption — a process essential for calcium mobilization. Simultaneously, 1,25(OH)2D promotes osteoblast synthesis of osteocalcin and osteopontin, supporting bone matrix mineralization. The net effect depends on calcium status: under adequate calcium, vitamin D favors bone formation; under deficiency, it mobilizes skeletal calcium stores (PMID: 22536764).
Immunomodulatory Effects
VDR is expressed in most immune cells. In macrophages, 1,25(OH)2D2 induces cathelicidin (LL-37) antimicrobial peptide expression. It suppresses Th1 pro-inflammatory cytokines (IL-2, IFN-gamma) while promoting Th2 and regulatory T-cell responses, contributing to immune tolerance (PMID: 21527855).
Reconstitution Calculator
Reconstitution Calculator
Calculate your peptide dosing

Set up a clean workspace with all supplies ready.
7x / week for weeks
Research
Reported Effects
Lower Efficacy vs D3:: Multiple studies and user reports confirm D2 is less effective than D3 at raising and maintaining serum vitamin D levels. Requires Higher Doses:: Users often need higher or more frequent doses of D2 compared to D3 to achieve the same blood level improvements. Variable Absorption:: Some users report D2 fails to correct deficiency even at high prescription doses (50,000 IU weekly), possibly due to cofactor deficiencies. Best for Severe Deficiency:: Most effective when used short-term to correct severe deficiency, then switching to daily D3 for maintenance
- Multiple studies and user reports confirm D2 is less effective than D3 at raising and maintaining serum vitamin D levels
- Users often need higher or more frequent doses of D2 compared to D3 to achieve the same blood level improvements
- Some users report D2 fails to correct deficiency even at high prescription doses (50,000 IU weekly), possibly due to cofactor deficiencies
- Most effective when used short-term to correct severe deficiency, then switching to daily D3 for maintenance
Safety Profile
Safety Profile: Ergocalciferol (Vitamin D2)
Common Side Effects
- Gastrointestinal symptoms: nausea, vomiting, constipation, metallic taste
- Headache and fatigue with supratherapeutic doses
- Mild hypercalcemia symptoms: increased thirst, frequent urination, dry mouth
- Weakness and muscle aches during dose adjustment
- Loss of appetite at higher doses
Serious Adverse Effects
- Hypercalcemia: Elevated serum calcium leading to confusion, cardiac arrhythmias, polyuria, polydipsia, and renal impairment; can be life-threatening
- Hypercalciuria and nephrolithiasis: Calcium-containing kidney stones with chronic high-dose supplementation
- Nephrocalcinosis: Calcium deposition in renal tissue with prolonged toxicity
- Cardiovascular calcification: Vascular and soft-tissue calcification with sustained hypercalcemia
- Acute kidney injury: Secondary to severe hypercalcemia
- Pancreatitis: Rare, associated with severe hypercalcemia
Contraindications
- Hypercalcemia (serum calcium > 10.5 mg/dL)
- Hypervitaminosis D
- Known hypersensitivity to ergocalciferol or vitamin D analogs
- Malabsorption syndromes may require alternative forms (parenteral or calcifediol)
- Severe hyperphosphatemia without phosphate management
Drug Interactions
- Thiazide diuretics (hydrochlorothiazide): Reduce renal calcium excretion; combined use increases hypercalcemia risk
- Cardiac glycosides (digoxin): Hypercalcemia potentiates digoxin toxicity; monitor calcium and digoxin levels closely
- Corticosteroids (prednisone): Antagonize vitamin D effects by reducing calcium absorption; may require higher vitamin D doses
- Cholestyramine and orlistat: Reduce vitamin D absorption; space dosing by 2-4 hours
- Anticonvulsants (phenytoin, phenobarbital): Increase vitamin D catabolism via CYP450 induction; supplementation doses may need to be higher
- Calcium supplements: Additive hypercalcemia risk; monitor total calcium intake
- Magnesium-containing antacids: Risk of hypermagnesemia in renal impairment patients
Population-Specific Considerations
- Elderly: Higher risk of hypercalcemia due to reduced renal clearance; start with lower doses and monitor 25(OH)D and calcium levels
- Pediatric: Safe within recommended daily allowances (400-600 IU/day); toxicity risk with accidental overdose
- Renal impairment: Impaired conversion to active 1,25(OH)2D; may require calcitriol instead; monitor phosphate and calcium
- Pregnant women: Safe at recommended doses (600-800 IU/day); high doses (>4000 IU/day) may cause fetal hypercalcemia
- Breastfeeding: Supplementation generally recommended (600 IU/day); high maternal doses transfer to breast milk
- Granulomatous diseases (sarcoidosis, TB): Extrarenal 1-alpha-hydroxylase activity increases toxicity risk; use with close monitoring
- Obese patients: May require 2-3x standard doses due to sequestration in adipose tissue
Pharmacokinetic Profile
Molecular Structure
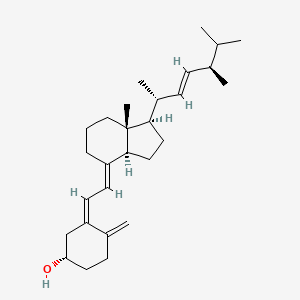
- Formula
- C28H44O
- Weight
- 396.6 Da
- PubChem CID
- 5280793
- Exact Mass
- 396.3392 Da
- LogP
- 7.4
- TPSA
- 20.2 Ų
- H-Bond Donors
- 1
- H-Bond Acceptors
- 1
- Rotatable Bonds
- 5
- Complexity
- 678
Identifiers (SMILES, InChI)
InChI=1S/C28H44O/c1-19(2)20(3)9-10-22(5)26-15-16-27-23(8-7-17-28(26,27)6)12-13-24-18-25(29)14-11-21(24)4/h9-10,12-13,19-20,22,25-27,29H,4,7-8,11,14-18H2,1-3,5-6H3/b10-9+,23-12+,24-13-/t20-,22+,25-,26+,27-,28+/m0/s1
MECHNRXZTMCUDQ-RKHKHRCZSA-NSafety Profile
Common Side Effects
- Poor Absorption:: Many users report D2 fails to raise blood levels adequately even at high doses, suggesting absorption issues
- Requires Cofactors:: Without magnesium and K2, users report side effects like muscle twitches, anxiety, and calcium distribution problems
- Weekly Dosing Issues:: Large weekly doses may cause fluctuating levels rather than stable daily levels, potentially affecting efficacy
- Individual Variation:: Some users respond poorly to D2 while responding well to D3, suggesting metabolic differences in processing the two forms
References (2)
- [1]Relative Efficacy of Vitamin D2 and Vitamin D3 in Improving Vitamin D Status: Systematic Review and Meta-Analysis
→ Meta-analysis found that vitamin D3 (cholecalciferol) is more effective than vitamin D2 (ergocalciferol) at raising and maintaining serum 25-hydroxyvitamin D levels, with D3 showing superior efficacy in correcting vitamin D deficiency.
- [2]Cholecalciferol v. Ergocalciferol for 25-hydroxyvitamin D (25(OH)D) repletion in chronic kidney disease: a randomised clinical trial
→ Randomized trial in chronic kidney disease patients demonstrated that cholecalciferol (D3) was significantly more effective than ergocalciferol (D2) for achieving target vitamin D levels and maintaining them over time.