Substance P
Substance P is an 11-amino acid tachykinin neuropeptide that functions as a key neurotransmitter in pain transmission, neurogenic inflammation, and mood regulation through the neurokinin-1 (NK1) receptor. It is one of the most extensively studied neuropeptides and the target of NK1 receptor antagonists used clinically as antiemetics.
Substance P is an undecapeptide (11 amino acids) belonging to the tachykinin neuropeptide family, first identified by Ulf von Euler and John Gaddum in 1931 as an uncharacterized substance in equine brain and intestinal extracts that caused smooth muscle contraction. Its full sequence was determined by Susan Leeman and Michael Chang in 1971, revealing the characteristic C-terminal Phe-X-Gly-Leu-Met-NH₂ motif shared by all mammalian tachykinins.
Overview
Substance P is encoded by the preprotachykinin A (TAC1) gene, which also produces neurokinin A (NKA) through alternative splicing. It is widely distributed throughout the central and peripheral nervous systems, with particularly dense expression in dorsal root ganglion neurons (small-diameter C fibers), the spinal cord dorsal horn (laminae I and II), the brainstem (nucleus tractus solitarius, area postrema), and limbic structures (amygdala, hypothalamus, periaqueductal gray).
Substance P preferentially binds the neurokinin-1 (NK1) receptor, a Gq-coupled GPCR, with secondary activity at NK2 and NK3 receptors. Through NK1 receptor activation, substance P mediates pain transmission at the first spinal synapse, triggers neurogenic inflammation (vasodilation, plasma extravasation, immune cell recruitment), modulates emesis via brainstem circuits, and influences mood and stress responses through limbic signaling (Steinhoff et al., 2014).
The discovery that NK1 receptor antagonists could block chemotherapy-induced nausea led to the approval of aprepitant (Emend) in 2003, validating substance P as a drug target. However, NK1 antagonists failed to demonstrate consistent analgesic efficacy in human pain trials despite strong preclinical evidence, highlighting the complexity of translating neuropeptide biology to therapeutics.
Mechanism of Action
Substance P's diverse biological effects are mediated primarily through NK1 receptor signaling:
- NK1 receptor activation (Gq/11-coupled): Binding activates phospholipase C, generating IP3 (calcium release) and DAG (PKC activation). This drives neuronal excitation, smooth muscle contraction, and glandular secretion. In the spinal dorsal horn, NK1 receptor activation on projection neurons amplifies and sustains nociceptive signaling, contributing to central sensitization and wind-up (Mantyh, 2002).
- Pain transmission: Substance P is co-released with glutamate from primary afferent C fiber terminals in the spinal cord lamina I. While glutamate mediates fast excitatory transmission, substance P produces slow, sustained depolarization via NK1 receptors, amplifying pain signals during prolonged or intense stimulation. Ablation of NK1 receptor-expressing neurons in lamina I profoundly reduces chronic pain behaviors in animal models (Nichols et al., 1999).
- Neurogenic inflammation: Peripheral substance P release from sensory nerve terminals (antidromic release) triggers the classic neurogenic inflammatory triad: arteriolar vasodilation, venular plasma protein extravasation, and mast cell degranulation. This mechanism contributes to inflammatory pain, migraine, asthma, and inflammatory bowel disease (Richardson & Vasko, 2002).
- Emesis: Substance P/NK1 signaling in the nucleus tractus solitarius and area postrema mediates the emetic reflex, particularly in response to chemotherapy agents and vagal afferent stimulation. NK1 receptor antagonists (aprepitant, fosaprepitant) block this pathway.
- Mood and stress: Substance P is released in the amygdala and hypothalamus during stress, and NK1 receptor activation promotes anxiety-like and depressive behaviors in animal models. Elevated CSF substance P levels correlate with depression severity in some studies (Bondy et al., 2003).
Reconstitution Calculator
Substance P
**Substance P** is an undecapeptide (11 amino acids) belonging to the tachykinin

Set up a clean workspace with all supplies ready.
7x / week for weeks
Research
Mood Disorders and NK1 Antagonists
Early clinical trials of the NK1 antagonist MK-869 (aprepitant) showed antidepressant efficacy comparable to paroxetine, generating enormous interest in substance P as a target for mood disorders (Kramer et al., 1998). However, subsequent larger trials produced inconsistent results, and NK1 antagonists have not been approved for depression. Research continues on the relationship between substance P, stress neurocircuitry, and affective disorders, with evidence suggesting NK1 receptor roles in stress resilience and anxiety (Ebner & Singewald, 2006).
Antiemetic Therapy (NK1 Antagonists)
The most successful clinical translation of substance P biology is in emesis control. Aprepitant (Emend, FDA approved 2003) and its IV prodrug fosaprepitant are standard components of antiemetic regimens for highly emetogenic chemotherapy (cisplatin). The CINV (chemotherapy-induced nausea and vomiting) indication validated the substance P/NK1 pathway in humans. Newer NK1 antagonists (rolapitant, netupitant in the fixed combination NEPA) have extended the class with improved pharmacokinetics (Hesketh et al., 2003).
Immune Modulation
Substance P modulates immune function through NK1 receptors on macrophages, T lymphocytes, dendritic cells, and mast cells. It promotes pro-inflammatory cytokine release (TNF-alpha, IL-1, IL-6), enhances T cell proliferation, and stimulates immunoglobulin production. In the gut, substance P from enteric neurons and immune cells contributes to mucosal inflammation in IBD. This neuroimmune interface represents an active research frontier (Mashaghi et al., 2016).
Pain Transmission and Central Sensitization
Substance P's role in pain is most significant in chronic and inflammatory pain states rather than acute nociception. During sustained C fiber activation, substance P release produces slow EPSPs that summate to produce "wind-up" — progressive amplification of dorsal horn neuron firing. NK1 receptor-expressing projection neurons in lamina I relay this amplified signal to supraspinal pain centers. Mantyh et al. (1997) demonstrated that selective destruction of lamina I NK1 receptor-expressing neurons with substance P-saporin conjugate abolishes hyperalgesia and allodynia without affecting acute pain responses (Mantyh et al., 1997).
Despite robust preclinical evidence, NK1 receptor antagonists (aprepitant, casopitant, orvepitant) have consistently failed to demonstrate analgesic efficacy in human clinical pain trials. This translational failure has been attributed to species differences in NK1 receptor pharmacology, redundancy in pain pathways, and the possibility that substance P's pain role is more modulatory than essential in humans (Hill, 2000).
Neurogenic Inflammation
Substance P is a principal mediator of neurogenic inflammation, the process by which sensory nerve activation directly drives tissue inflammation independent of immune cells. Upon C fiber stimulation, substance P is released antidromically from peripheral nerve terminals, causing arteriolar vasodilation (via endothelial NO release), venular plasma extravasation (via endothelial cell contraction), and mast cell degranulation (histamine release). This mechanism contributes to inflammatory conditions including arthritis, asthma, psoriasis, and inflammatory bowel disease (O'Connor et al., 2004).
Safety Profile
Substance P itself is not administered therapeutically; rather, its receptor (NK1) is a pharmacological target for antagonist drugs. Endogenous substance P dysregulation is implicated in pathological states including chronic pain, neurogenic inflammation, and mood disorders. NK1 receptor antagonists (aprepitant class) have a favorable safety profile with common side effects including fatigue, hiccups, and constipation. Aprepitant is a moderate CYP3A4 inhibitor and CYP2C9 inducer, requiring attention to drug interactions (particularly with dexamethasone dosing and warfarin monitoring). No significant safety concerns have been identified with short-course antiemetic use. Long-term NK1 antagonist exposure data remain limited.
Pharmacokinetic Profile
Substance P — Pharmacokinetic Curve
Molecular Structure
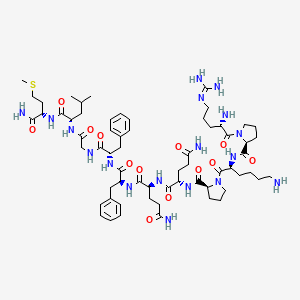
- Formula
- C₆₃H₉₈N₁₈O₁₃S
- Weight
- 1347.6 Da
- CAS
- 33507-63-0
- PubChem CID
- 36511
- Exact Mass
- 1346.7281 Da
- LogP
- -2.3
- TPSA
- 544 Ų
- H-Bond Donors
- 15
- H-Bond Acceptors
- 17
- Rotatable Bonds
- 42
- Complexity
- 2620
Identifiers (SMILES, InChI)
InChI=1S/C63H98N18O13S/c1-37(2)33-45(57(89)74-41(53(68)85)27-32-95-3)73-52(84)36-72-54(86)46(34-38-15-6-4-7-16-38)78-58(90)47(35-39-17-8-5-9-18-39)79-56(88)42(23-25-50(66)82)75-55(87)43(24-26-51(67)83)76-59(91)49-22-14-31-81(49)62(94)44(20-10-11-28-64)77-60(92)48-21-13-30-80(48)61(93)40(65)19-12-29-71-63(69)70/h4-9,15-18,37,40-49H,10-14,19-36,64-65H2,1-3H3,(H2,66,82)(H2,67,83)(H2,68,85)(H,72,86)(H,73,84)(H,74,89)(H,75,87)(H,76,91)(H,77,92)(H,78,90)(H,79,88)(H4,69,70,71)/t40-,41-,42-,43-,44-,45-,46-,47-,48-,49-/m0/s1
ADNPLDHMAVUMIW-CUZNLEPHSA-NResearch Indications
Neurological
Key neuropeptide in pain transmission via NK1R at the spinal cord dorsal horn. Implicated in central sensitization and chronic pain transition. Extensive preclinical and human biomarker evidence (PMC6335504).
Contributes to trigeminovascular neurogenic inflammation via vasodilation, plasma protein extravasation, and mast cell degranulation. NK1R antagonists investigated as antimigraine agents (PMID: 40746227).
NK1R antagonists studied for antidepressant and anxiolytic effects. Preclinical and clinical evidence supports SP/NK1R involvement in mood disorders. Phase II/III trials of NK1R antagonists.
Immune
Modulates immune cell proliferation and cytokine production via NK1R. Biases inflammatory response toward Th17 immunity and regulates Th1/Th2 balance (PMC5056132).
SP/NK1R signaling implicated in GI inflammation. NK1R antagonists investigated for IBD therapy. Preclinical evidence in colitis models.
Dermatological
SP-derived peptides with IGF-1 successfully treated persistent corneal epithelial defects and neurotrophic keratopathy in clinical trials. Promotes angiogenesis and tissue repair (PMC5657331).
Interactions
Peptide Interactions
Substance P and CGRP are co-stored in peptidergic C-fibers and co-released during neurogenic inflammation via the axon reflex. CGRP potentiates SP-induced plasma protein extravasation by inhibiting SP degradation through competition for the same endopeptidase (Brain & Williams, 1988). In temporal muscle, CGRP alone does not induce pain but synergistically elicits significant pain sensation when combined with SP (Arendt-Nielsen et al., 1992). Together they mediate the neurogenic inflammatory response: SP causes plasma extravasation while CGRP provides potent vasodilation.
Bradykinin stimulates release of Substance P from sensory nerve terminals, creating a positive feedback loop in neurogenic inflammation. Both peptides are key mediators of pain and inflammation, with bradykinin acting via B1/B2 kinin receptors and Substance P via NK1 receptors. Dual blockade of kinin and neurokinin pathways may provide superior anti-inflammatory effects (Geppetti et al., 1990).
Somatostatin and Substance P are co-expressed in enteric neurons and have opposing modulatory roles — SP is excitatory/pro-nociceptive while somatostatin is inhibitory. In the dorsal horn, somatostatin modulates pain signaling alongside SP. They compete for similar metabolic degradation pathways. No dangerous interactions; they represent complementary regulatory mechanisms in the gut and sensory nervous system.
Opioid peptides including beta-endorphin functionally counteract Substance P signaling. Presynaptic activation of opioid receptors in the dorsal horn inhibits the release of both glutamate and Substance P, reducing ascending pain signal transmission. CSF studies show a highly significant positive correlation between SP and met-enkephalin levels in chronic pain states (Almay et al., 1988). These peptides represent opposing arms of pain modulation and are physiologically safe together.
SP and VIP are co-localized in enteric neurons, with differential expression patterns — SP predominantly in the myenteric plexus and VIP in the submucous plexus. They have complementary roles in gastrointestinal motility and secretion. Both participate in neuroimmune regulation, with VIP generally anti-inflammatory and SP pro-inflammatory. No adverse interactions reported; they represent balanced neuromodulation.
What to Expect
What to Expect
Rapid onset expected; half-life of ~1-2 minutes (plasma) indicates fast-acting pharmacokinetics
Due to short half-life (~1-2 minutes (plasma)), effects are expected per-dose; consistent daily administration maintains therapeutic levels
Regular administration schedule required; effects are dose-dependent and do not persist between doses
Quality Indicators
What to look for
- Well-established safety profile
- Extensive peer-reviewed research base
- Extensive preclinical data
Frequently Asked Questions
References (13)
- [1]Steinhoff MS et al Tachykinins and their receptors: contributions to physiological control and the mechanisms of disease Physiol Rev (2014)
- [7]Hill R NK1 (substance P) receptor antagonists — why are they not analgesic in humans? Trends Pharmacol Sci (2000)
- [5]
- [2]
- [3]Nichols ML et al Transmission of chronic nociception by spinal neurons expressing the substance P receptor Science (1999)
- [4]Mantyh PW et al Inhibition of hyperalgesia by ablation of lamina I spinal neurons expressing the substance P receptor Science (1997)
- [6]Kramer MS et al Distinct mechanism for antidepressant activity by blockade of central substance P receptors Science (1998)
- [8]Hesketh PJ et al The oral neurokinin-1 antagonist aprepitant for the prevention of chemotherapy-induced nausea and vomiting J Clin Oncol (2003)
- [9]Bondy B et al Substance P serum levels are increased in major depression: preliminary results Biol Psychiatry (2003)
- [10]
- [11]
- [12]
- [13]Munoz M, Covenas R The neurokinin-1 receptor antagonist aprepitant: an intelligent bullet against cancer? Cancers (2020)
Stamakort
Stamakort is a complex peptide bioregulator preparation derived from gastric mucosal tissue, developed for targeted support of stomach function and gastrointestinal mucosal integrity. Research indicates potential gastroprotective effects including reduced mucosal inflammation, enhanced epithelial repair, and improved gastric secretory function in aging models.
Super Human Blend (CJC-1295 + Ipamorelin + BPC-157 + TB-500)
The Super Human Blend is a compounded four-peptide combination of CJC-1295 (GHRH analog), Ipamorelin (GH secretagogue), BPC-157 (tissue repair peptide), and TB-500 (thymosin beta-4 fragment). The protocol combines growth hormone secretagogues with healing peptides for a multi-pathway approach to recovery, body composition, and regeneration.